A traumatic brachial plexus injury (TBPI) is one of the most severe and devastating injuries an individual can experience. Although less well-known than spinal cord or brain injuries, the consequences can be every bit as life-altering. These injuries often follow high‑energy trauma, frequently in the context of road traffic collisions. They can leave individuals facing profound physical limitations, chronic pain and significant disruption to their daily lives, careers and future plans.
In this article, injury partner Scott Rigby explains what the brachial plexus is, how traumatic injuries occur and why living with a brachial plexus injury presents such significant challenges. He also sets out information about Stewarts’ free legal service for members of the Traumatic Brachial Plexus Injury Group.
What is the brachial plexus?
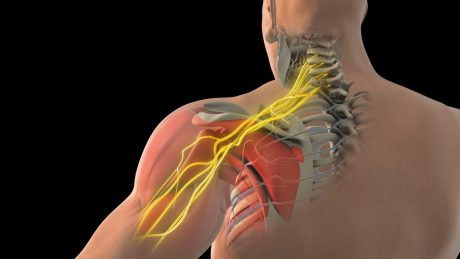
The brachial plexus is a complex network of nerves that originates from the spinal cord in the neck (C5–T1). These nerves branch down through the shoulder and into the arm, controlling:
- movement of the shoulder, arm, elbow, wrist and hand
- sensation throughout the upper limb
- fine motor function, coordination and grip strength.
When these nerves are damaged, the ability to move, feel, and use the arm is impaired, sometimes partially, sometimes entirely.
What is a traumatic brachial plexus injury?
A traumatic brachial plexus injury occurs when the nerves are stretched, torn or avulsed (pulled directly from the spinal cord) due to a sudden, violent force. These injuries most commonly arise from:
- motorcycle collisions
- high‑impact road traffic accidents
- industrial or workplace incidents
- falls from height or sports accidents.
Unlike minor nerve injuries that may recover over time, a TBPI often results in serious, long‑term impairment. Avulsion injuries typically leave the affected limb paralysed.
How does a traumatic brachial plexus injury affect the body?
Because the brachial plexus provides both movement and sensation to the arm, damage can cause a range of life‑changing symptoms:
Paralysis or loss of movement
Depending on which nerves are affected, a person may lose the ability to:
- lift the arm
- bend the elbow
- move the wrist
- open or close the hand.
In the most severe injuries, the entire arm becomes a flail limb, with no active movement at all.
Loss of sensation
A TBPI often causes numbness, altered sensation or complete loss of feeling. This can make everyday tasks dangerous. Burns, cuts and injuries can occur without the person noticing.
Severe neuropathic pain
Neuropathic pain is one of the hallmark challenges of TBPI. Individuals often report:
- burning
- pins and needles
- electric shock sensations
- deep, constant aching or stabbing pain.
This pain can be debilitating and is notoriously difficult to treat.
Muscle wasting and postural changes
When nerves cannot activate muscles, the muscles weaken and waste away over time. The shoulder may become unstable, visibly altering posture and symmetry.
What is the diagnosis, treatment and rehabilitation for a traumatic brachial plexus injury?
Early specialist assessment
Prompt referral to a specialist brachial plexus centre is essential. Diagnosis typically involves:
- MRI or CT myelography
- electromyography (EMG) and nerve conduction studies
- clinical assessment by an upper‑limb nerve specialist.
Early intervention maximises the chance of meaningful recovery.
Surgical options
Treatment depends on the pattern of nerve damage. Options may include:
- nerve grafts
- nerve transfers (borrowing nerves from other areas of the body)
- muscle or tendon transfers
- joint fusion procedures for stability.
These surgeries are highly specialist and often time‑critical, typically performed within the first six months post‑injury.
Rehabilitation
Rehabilitation is a long‑term process requiring:
- specialist physiotherapy
- occupational therapy
- pain management
- adaptive equipment
- psychological support.
Even with surgery and comprehensive rehabilitation, full recovery is rare. Many individuals live with permanent impairment.
The human impact: challenges of living with a TBPI
Loss of independence
Everyday tasks such as washing, dressing, cooking and carrying objects often require new techniques or support. Activities once taken for granted may become frustrating or exhausting.
Driving and mobility
Many people cannot drive for months or longer, and may need:
- specialist medical clearance
- vehicle adaptations
- retraining or assessment.
This loss of mobility affects work, childcare, and social independence.
Work and financial consequences
Because TBPIs frequently affect younger, active individuals, including motorcyclists, tradespeople and engineers, the impact on employment can be profound. Many cannot return to their previous roles. This may mean:
- loss of income
- the need for retraining
- a change in career altogether
- increased household financial pressure.
Pain, fatigue and sleep disturbance
Neuropathic pain can be relentless, affecting concentration, mood and sleep. Chronic sleep disruption contributes to fatigue and emotional strain.
Changes in body image and confidence
Visible changes, such as muscle wasting, scarring and altered posture, can affect confidence and willingness to engage socially.
Emotional and psychological adjustment
Living with a TBPI often involves a process of grief and adaptation. Individuals may experience:
- frustration
- anxiety
- low mood
- loss of identity, particularly around work or hobbies.
Support from clinicians, family, peers and specialist groups is essential.
Support, advocacy and access to specialist legal help
For many people, navigating life after a traumatic brachial plexus injury is overwhelming. Access to early rehabilitation, specialist medical input, financial security and emotional support can make an enormous difference to long‑term outcomes. This is why clear, compassionate legal guidance is essential when the injury results from an accident caused by another party’s fault.
Over the years, Stewarts has worked with many people living with traumatic brachial plexus injuries. The impact on their independence, work, identity and day‑to‑day life is profound. That’s why early, accessible legal support is so important. The goal of Stewarts’ free legal service for members of the Traumatic Brachial Plexus Injury Group is to ensure that no one faces this journey alone and that every individual has the chance to access the rehabilitation, financial security and long‑term support they need to rebuild their lives.
This free service ensures that individuals and families can quickly understand their rights, the potential for rehabilitation funding and the legal steps available to secure long‑term support, without any barriers to initial advice.
Conclusion
Traumatic brachial plexus injuries are severe and complex, affecting far more than the physical function of the arm. They can reshape every part of an individual’s life, from work and independence to emotional well-being and identity. Yet with specialist treatment, early intervention and strong support, many people rebuild independence and adapt in meaningful ways.
Raising awareness of TBPIs helps ensure that those affected receive the understanding, specialist attention and long‑term support they need.
Find out more
You can find further information regarding our expertise, experience and team on our Personal Injury page.
If you require assistance from our team, please contact us.